Menopause and Osteoporosis
Explanation
Osteoporosis is a condition where bones become weaker, thinner, and more prone to fractures. During menopause, declining estrogen levels accelerate bone loss, making osteoporosis a major health concern for women in midlife and beyond. Many women don’t realize they have osteoporosis until they experience a fracture, often in the spine, hip, or wrist.
Causes and Risk Factors
Estrogen helps maintain bone density by slowing the natural breakdown of bone. With menopause, bone resorption outpaces bone formation. Additional risk factors include:
Age (bone loss accelerates after menopause, especially in the first 5–7 years)
Family history of osteoporosis or fractures
Low body weight or small frame
Lack of calcium and vitamin D
Smoking or heavy alcohol use
Sedentary lifestyle
Certain medications (e.g., corticosteroids, cancer treatments)
Early menopause or surgical removal of ovaries
Linked Health Conditions
Osteoporosis is often connected with or increases risk for:
Bone fractures – especially hips, wrists, and vertebrae
Spinal deformities – such as stooped posture or loss of height
Chronic pain – from fractures or vertebral compression
Reduced mobility and independence
Higher risk of falls – due to muscle weakness or balance issues
Diagnosis and Treatment
Osteoporosis is often called a “silent disease” because it develops without symptoms until a fracture occurs. Diagnosis may include:
Bone density testing (DEXA scan) – the gold standard for diagnosing osteoporosis
Blood and urine tests – to rule out secondary causes
Fracture risk assessments – tools like FRAX to estimate future risk
Treatment options include:
Medications: Bisphosphonates, hormone therapy (HRT), selective estrogen receptor modulators (SERMs), or newer bone-building drugs
Calcium and vitamin D supplements – to support bone strength
Lifestyle changes: Exercise, nutrition, and smoking cessation
Fall prevention strategies: Home safety modifications, balance training
Preventative Lifestyle Measures
The good news is that osteoporosis risk can be managed with proactive choices:
Eat for bone health: Calcium-rich foods (dairy, leafy greens, fortified products) and vitamin D (sunlight, fatty fish, eggs)
Exercise regularly: Weight-bearing activities (walking, dancing, jogging) and strength training to stimulate bone growth
Avoid smoking and excess alcohol: Both accelerate bone loss
Maintain a healthy weight: Extremely low or high body weight increases risk
Protect against falls: Improve home safety, wear supportive footwear, and practice balance exercises like yoga or tai chi
Regular screenings: DEXA scans starting around menopause, or earlier if risk factors are present
Managing Osteoporosis
-
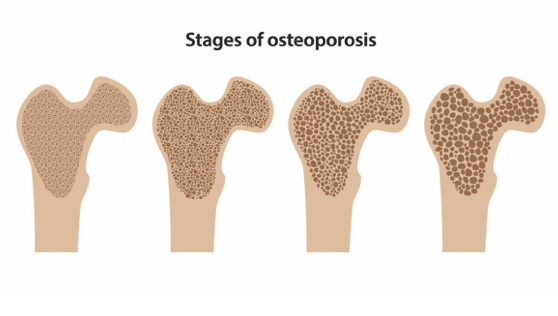
How to Prevent Osteoporosis after Menopause
How to prevent osteoporosis during perimenopause and how to treat it after menopause
-
Post Menopausal Osteoporosis
How to treat it, how to best prevent it, and how to assess your risk factors
-
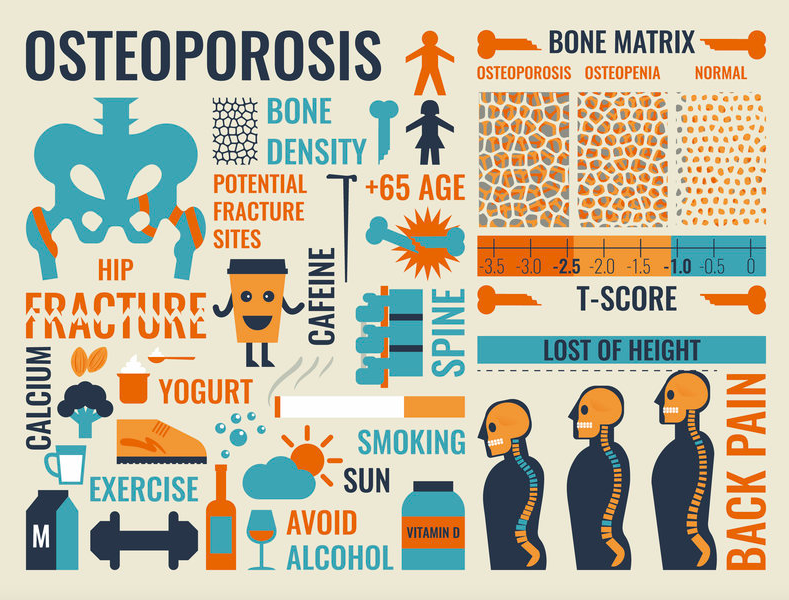
Lifestyle for Healthy Bones
Exercises, diet, and lifestyle modifications to help maintain bone health throughout the years