Menopause and Headaches
Explanation
Headaches are a frequent symptom during the menopause transition. Many women notice increased frequency or intensity of headaches, including tension-type headaches or migraines. These can be triggered by hormonal fluctuations, particularly estrogen, which influences blood vessels, brain chemicals, and pain pathways.
Causes and Risk Factors
Menopausal headaches are most often linked to changing estrogen and progesterone levels, but other contributing factors include:
Perimenopausal hormone fluctuations
Poor sleep or insomnia (often due to night sweats or hot flashes)
High stress and elevated cortisol
Caffeine withdrawal or overuse
Dehydration and skipped meals
Certain foods (aged cheeses, processed meats, alcohol, chocolate)
Genetics and history of migraines
Linked Health Conditions
Headaches during menopause may overlap with or increase risk for:
Migraines – often worsen during perimenopause, then improve postmenopause
Tension headaches – linked with stress, muscle tightness, and poor posture
Sleep disorders – headaches are commonly associated with insomnia and disrupted rest
Depression and anxiety – mental health conditions can amplify pain perception
Cardiovascular concerns – migraines with aura may increase stroke risk in midlife women
Diagnosis and Treatment
Diagnosis of menopausal headaches is based on symptom history and ruling out other causes. Steps may include:
Medical history and symptom tracking – including cycle patterns, triggers, and headache type
Physical and neurological exams – to assess for underlying conditions
Blood tests or imaging – if severe or unusual symptoms occur
Treatment options include:
Hormone therapy (HRT): May stabilize headaches for some women but can worsen migraines in others
Medications: NSAIDs, triptans, or preventive migraine medications when needed
Lifestyle adjustments: Consistent sleep, hydration, stress management, and trigger avoidance
Alternative therapies: Acupuncture, massage, biofeedback, or magnesium supplements
Preventative Lifestyle Measures
Daily habits can help reduce the frequency and severity of menopausal headaches:
Maintain regular sleep routines – avoid late nights and screen exposure before bed
Stay hydrated – dehydration is a common trigger
Eat balanced meals – avoid long fasting periods and trigger foods
Exercise regularly – aerobic activity improves circulation and reduces stress
Manage stress effectively – meditation, journaling, yoga, or breathwork
Limit alcohol and caffeine – to reduce both triggers and rebound headaches
Track symptoms – keeping a headache diary helps identify personal triggers
Resources for Headaches
-

Headache Journal
A place to write down symptoms, timing, interventions and see patterns over time.
-

Headaches and Menopause
The connection between menopause and headaches, migraines, and some helpful guidance on managing them
-
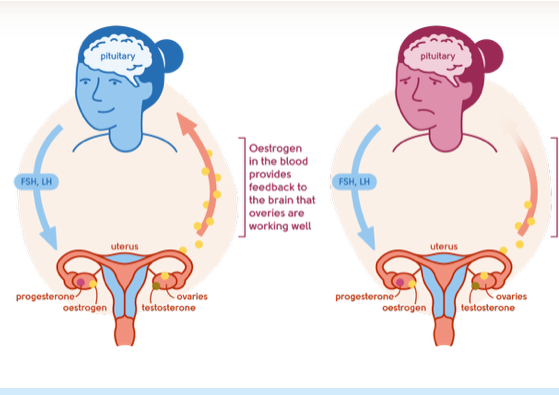
Menopause, headaches, and migraines
Identifying headaches and triggers to help manage symptoms and onsets